Rubella (German Measles): Symptoms,
Causes and Treatment
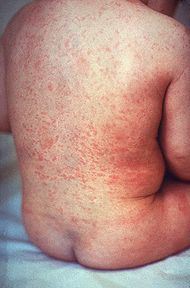
Rubella (German measles) is caused by the rubella virus. The name rubella is derived from the Latin meaning little red. Rubella is also known as German measles because the disease was first described by German physicians.
Rubella is such a mild disease that, if it werent for the severe complications caused to unborn babies, a vaccine wouldnt even have been developed.
Rubella symptoms usually last only about 3 days. The most characteristic of these being the fine red rash that develops.
HISTORY
Rubella was first described in the 18th century by Friedrich Hoffman, who made the first clinical description of the disease. In 1752 and 1758 this description was confirmed by de Bergen and Orlow, respectively.
George de Maton suggested, in 1814, that rubella be considered distinct from measles and scarlet fever. In 1881, rubella was officially recognized as an individual disease, and in 1914 it was first theorized that a virus causes the disease.
In 1940 an ophthalmologist, Norman McAllister Greg, found that 82% of babies born with congenital cataracts were born to mothers who had rubella during early pregnancy. Gregg also described a variety of complications, now known as congenital rubella syndrome (CRS). He noticed that the earlier the mother was infected with rubella, the worse the damage was.
In 1969 the first rubella virus was licensed and in the early 1970s the measles, mumps and rubella (MMR) vaccine was introduced.
INCUBATION AND CAUSES
Rubella has an incubation period of 14-21 days. During this time an infected person is contagious even if they show no symptoms. The person is also contagious for about 2 weeks after the rash disappears.
The virus breeds in the upper respiratory system (throat, nose etc.) and is spread through tiny airborne droplets of saliva or mucus.
The virus can also be spread through direct contact with these respiratory secretions, for example by touching an infected tissue.
The most dangerous form of transmission is from an expectant mother to her unborn baby.
SIGNS AND SYMPTOMS
The primary symptom is a rash that first appears on the face and then spreads to the body and limbs. The rash usually fades within 3 days, in the same sequence as it appeared.
Other symptoms could include:
- Mild fever (rarely above 38ºC).
- Swollen lymph nodes at the base of the scull, back of the neck and behind the ears.
- Mild headache.
- Conjunctivitis (inflamed, red eyes).
- Joint pain (especially in young women).
- Stuffy or runny nose.
The symptoms of rubella tend to be more severe in adults, but rubella is usually so mild that symptoms appear and disappear without even being noticed.
COMPLICATIONS
- CONGENITAL RUBELLA SYNDROME (CRS)
The rubella virus is capable of crossing the placenta. It infects the fetus where it stops cells from developing or destroys them altogether. If a mother is infected with rubella within the first 20 weeks of pregnancy, the baby could be born with what is known as CRS. CRS could cause congenital heart defects, deafness, organ defects, cataracts, or growth retardation. Eighty-five percent of babies born to mothers who had rubella during the first 20 weeks of pregnancy have CRS. In up to 20% of cases there is a spontaneous abortion (miscarriage) or still born baby.
- ARTHRITIS
Approximately 70% of young women with rubella experience arthritis in their joints. This lasts about a month, after which it disappears.
- OTITIS MEDIA AND ENCEPHALITIS
Rubella could cause secondary ear infections and encephalitis, but this is very rare.
DIAGNOSIS
A doctor will usually base a diagnosis on the symptoms presented. The rash is a key indicator of rubella. However, various other viral infections also present with a rash. For this reason, blood tests are usually also done in order to confirm the diagnosis.
TREATMENT
Since rubella is caused by a virus antibiotics cannot cure it. Treatment is therefore symptomatic:
- Sufficient bed rest and plenty of fluids are recommended.
- Pain and fever can be treated with paracetamol. Never give children and teens younger than 18 years old aspirin. The combination of aspirin and viral infections have been linked to Reye's syndrome, a potentially fatal condition.
CRS treatment is based on managing the complications. For example, congenital heart defects and cataracts can be corrected with surgery.
Pregnant women who contract rubella might be given antibodies called hyper-immune globulin to help fight the infection. This could reduce symptoms, but it does not reduce the infants risk of developing CRS.
PREVENTION
- People who have had rubella have life-long protection against contracting it again.
- Babies are protected after birth for about 6 months, because of immunity passed on from their mothers.
- MMR vaccination: the best way to prevent contracting rubella is by receiving 2 dosages of the MMR vaccine. The first dose is usually given to babies aged between 12 and 15 months and the second dose at around 18 months. A baby needs to receive both dosages in order to have sufficient protection against mumps, measles and rubella.
The vaccine is not recommended if:
- You are pregnant or plan to get pregnant within the next four weeks. The vaccine contains a live virus and this could infect the baby or cause a miscarriage.
- You have had a life threatening reaction to gelatin or the antibiotic neomycin.
- You have a weakened immune system (e.g. as a result of cancer or HIV/AIDS)
PROGNOSIS (OUTLOOK)
Rubella is usually mild and it can sometimes even go unnoticed. Adults and children who are infected usually make a full recovery within 3 days.
The prognosis for infants born with CRS is unfortunately poor. It is therefore vital to inform pregnant women if you have been diagnosed with the disease. Infected people should also preferably be kept away from, especially, pregnant women. Parents should also ensure that their children (especially girls) receive both MMR dosages.
Copyright 2009: Remedium. This article may not be copied, in whole or in part, without the written consent of Remedium.
|